Micro-incision Cataract Surgery with Artificial Lens Implantation
What is a cataract?
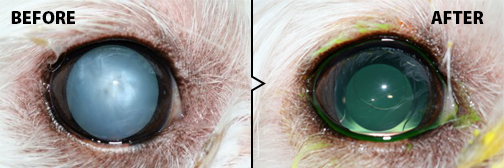
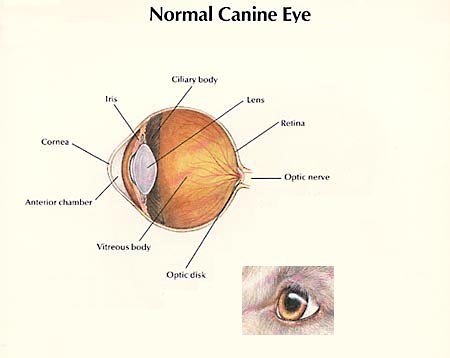
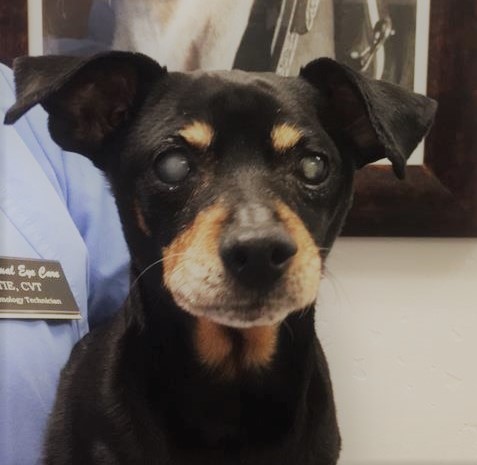
The lens of an animal should remain clear when healthy, this helps to focus light on the retina, a light-sensitive nervous tissue located at the back of the eye. A cataract develops when the lens hardens and becomes cloudy and opaque causing light to scatter. When most of the lens is cataractous, light cannot reach the retina, resulting in poor vision. Cataracts can have many appearances, from a small white dot to spiny white streaks. They can also affect only a small area, or the entire structure, as well as one or both eyes at the same or various times. Rate of progression is difficult to predict, though it tends to be more rapid in younger animals.
Causes
Many dogs cataracts are hereditary. Cataracts can also develop from injuries, inflammation, and systemic disease. Diabetes mellitus is the most common disease associated with cataracts in dogs. Eighty percent of dogs will develop cataracts within 18 months after being diagnosed with diabetes. Determining the exact underlying cause of the cataracts can be difficult, typically if they are formed in the absence of other signs or diseases and are considered inherited.
What does the surgery involve?
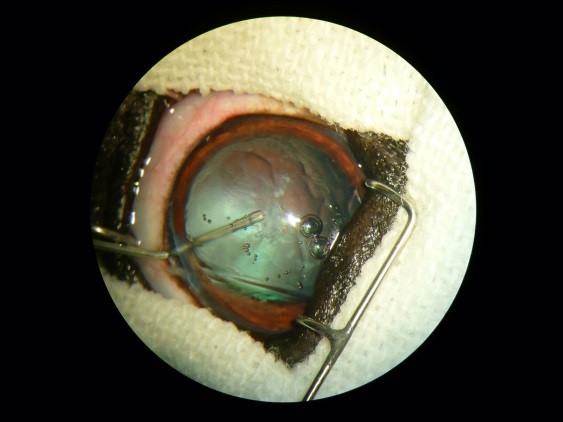
Cataract surgery is an outpatient procedure done under general anesthesia, occasionally a visit is required the following day. The same method used in people, phacoemulsification, is used in our pets. Through a microincision, ultrasonic waves from the instrument break up the cataract material and it is then aspirated out of the eye. Artificial lenses positioned to replace the cataract. This restores them to 20/20 vision, with no chance of cataract regrowth. The decision to place an intraocular lens in the eye may be affected by factors at the time of surgery. An eye in which an artificial lens cannot be placed will leave the eye far-sighted (objects far away are easily seen, closer objects are blurry), but still visual.
Post-Operative Care
After cataract surgery, pets usually require topical drops 3-4 times daily and 2-3 types of pills for a couple weeks, and then the frequency tapers down over 4-6 months to one drop once daily ongoing. Following surgery, there are typically 3-4 rechecks within the first few months after surgery to ensure success.
Possible Complications
Cataract surgery success has improved with the advent of newer medications and microsurgical techniques, but can vary with each patient. Minor complications may include uveitis (inflammation) within the eye, high pressure immediately after surgery, or a corneal ulcer. These complications may require additional visits and medications but will unlikely affect the long-term success rate. Major complications, or “failures”, may include retinal detachment or glaucoma, which are vision threatening and must be treated quickly. There is very minimal risk of infection in the eye following surgery although every precaution is taken to prevent infection. Together with your ophthalmologist, every effort is made to prevent complications from developing. However, if they occur these complications could result in the need for additional medications, more frequent re-examination, and permanent vision loss if the eye responds poorly to therapy.
Preparing for Surgery
Prior to surgery it is recommended that your pet have pre-operative lab work (CBC, Chemistry, Urinalysis) to ensure that the pet is an ideal candidate for surgery from an anesthesia standpoint, this can be done with your general practice veterinarian. Additional testing may be recommended if your pet is diabetic.
To better assess the eye and potential for vision, an Electroretinogram and ocular ultrasound will be performed either prior to or on the day of surgery.
· The electroretinogram (ERG) determines the electrical activity of the retina, similar to an electrocardiogram (ECG) for the heart. A normal ERG value suggests a healthy retina. A low ERG value can be a sign of retinal degeneration. Pets with retinal degeneration are likely to have poor vision (regardless of the presence or absence of cataracts).
· Ocular ultrasonography is a way to assess the position of the retina, in other words whether the retina is detached. Retinal detachments, which are often blinding, would mean poor candidacy for surgery.
Is Surgery the only option?
The decision to do surgery is based on the overall health of your pet, the effect of vision loss on their quality of life, and often the pet-owner’s finances; ultimately an individual’s choice. Together with your veterinary ophthalmologist, the pros and cons can be discussed. If cataract surgery is not elected, it is essential that all pets with cataracts are treated with topical drops to reduce the irritation that cataracts cause. Inflammation left untreated can cause painful secondary complications, such as glaucoma. They can also advise you on how to help your pet adapt to their vision loss.